Approximately 1/3 of all Positive Blood Cultures are FALSE Positive Blood Cultures
Research suggests that approximately 90% of all blood culture tests have negative results.1 That means that for every 1000 blood draws, about 100 patients receive a positive result. But, well-established false positive blood culture rates 2 tell us that ~30 of the patients who test positive do NOT have a bloodstream infection.
False positive blood culture results are common.
Positive blood culture results are WRONG ~1/3 of the time.
The Impact of False Positive Blood Culture Results
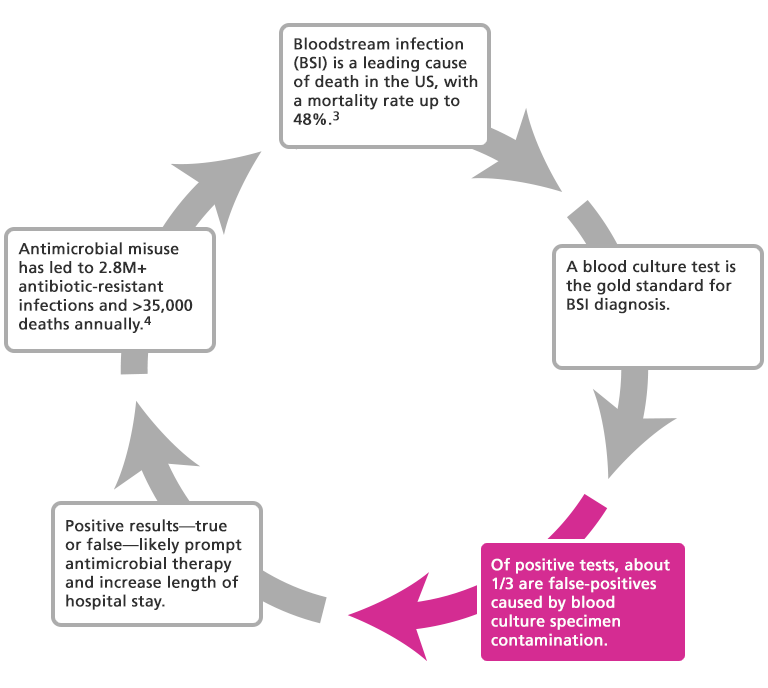
Blood culture contamination (BCC) that causes false positive results has consequences:
- Antibiotic misuse has led to life-threatening multi-drug resistant super bugs.
- Contaminated blood cultures put patients at higher risk of in-hospital mortality5, contribute to unnecessary antibiotic use and resistance, increase length of stay and associated healthcare-acquired conditions, and create delays in proper treatment.6
- The cost of a false-positive blood culture is estimated at $4,000-$10,0002,5,7,8, negatively impacting hospital financial performance.
- A new CMS law9 will penalize hospitals that are not demonstrating facility-wide antibiotic stewardship best practice, including avoiding unnecessary antibiotic use.





